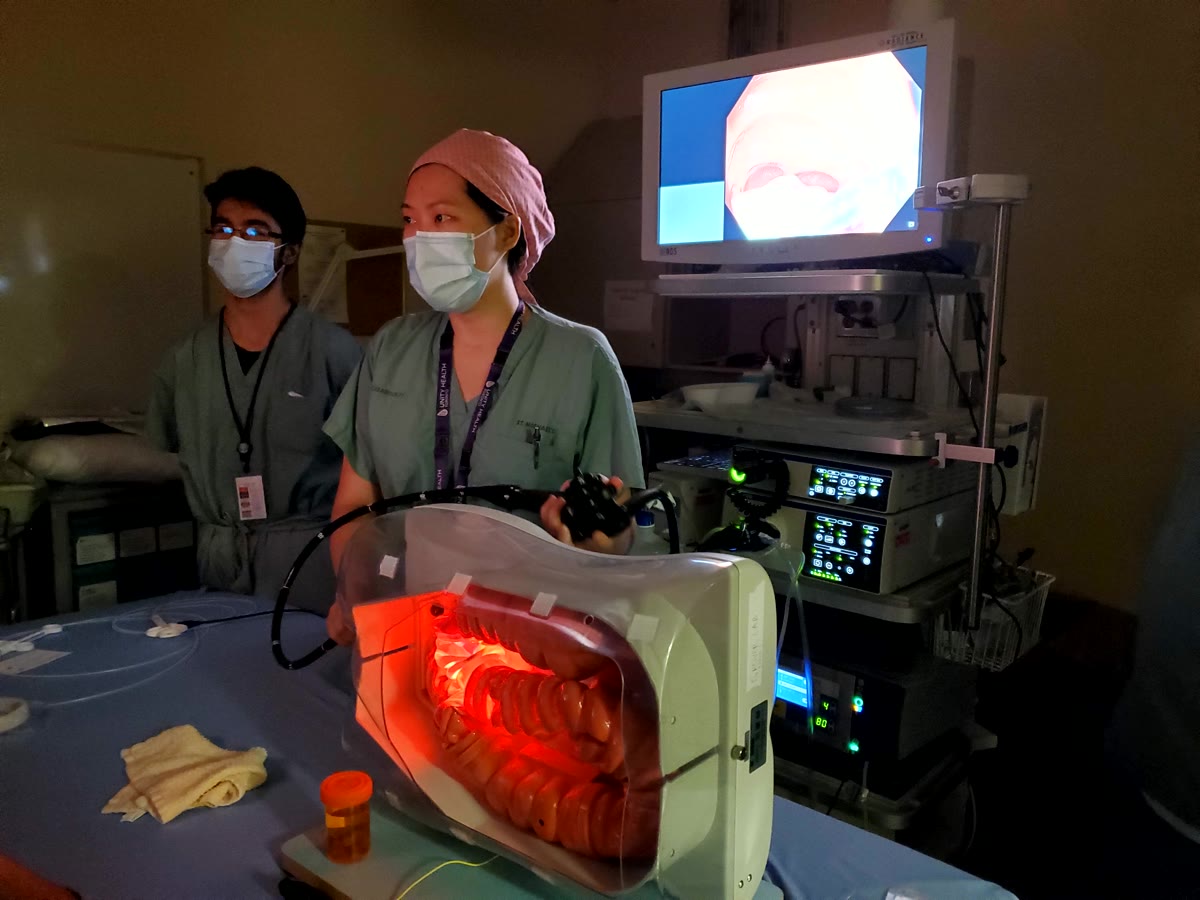
Why this area matters
Simulation lets educators increase deliberate practice without exposing patients to the learner’s earliest errors. But the value is not just safety. Good simulation can accelerate pattern recognition, procedural fluency, team communication, ergonomics, and self-assessment. It creates a place where repetition is possible, feedback is immediate, and curriculum can be structured around progression rather than chance exposure.
Grover Lab’s simulation work has focused on making training more frequent, more structured, more measurable, and more transferable to real clinical performance.
How Grover Lab approaches simulation
We have worked across multiple levels of the simulation stack: curriculum design, randomized trials, systematic reviews, low-cost simulator development, non-technical skills training, and ergonomics. The point is not simply to create a simulator. It is to build a training system around it. That includes deciding what sequence learners should follow, what feedback they should receive, how progression should occur, and how evidence of competence should be gathered.
This has led to a sustained body of work in endoscopy education, including progressive learning models, ergonomics curricula, non-technical skills training, and evidence synthesis around virtual reality simulation. It also connects naturally to current build-oriented work: as more of medical education becomes digitally instrumented, simulation and assessment start to converge.
What the program of work shows
Simulation improves performance when it is embedded in a curriculum. Our work has consistently treated simulation as part of a larger educational pathway rather than a one-off event.
Technical and non-technical skills both matter. Novices do not just need better scope handling or procedural sequencing. They also need communication, team awareness, ergonomics, and self-monitoring.
Low-cost and scalable models matter. Not every institution can buy the most sophisticated simulation suite. That makes low-cost model design and pragmatic educational strategy important, especially if the goal is wide adoption rather than isolated excellence.
Simulation links naturally to assessment. Once training is instrumented and structured, it becomes easier to collect meaningful signals about learner progress. That is one reason simulation work and performance-analytics work sit so close together in this lab.
Selected Grover Lab work in this area
Where this connects next
Simulation-based medical education does not sit apart from the lab’s newer AI and build work. It creates the conditions for better data, more structured performance measurement, and more defensible progression models. That is one reason the conversation increasingly overlaps with performance analytics, ambient assessment, and educational infrastructure.
If the AI page is about how training changes when models become part of the environment, this page is about a longer-standing truth: repeated, structured, feedback-rich practice is still how complex clinicians are formed.